What You Need to Know
If you’ve ever experienced painful periods, heavy bleeding, or pelvic pain, you might have wondered if there could be an underlying cause. One common condition that can lead to these symptoms is endometriosis. Although it affects millions of women worldwide, endometriosis is still widely misunderstood and under-diagnosed.

What is Endometriosis?
Endometriosis is a medical condition where tissue similar to the lining of the uterus (called the endometrium) grows outside the uterus. Normally, the endometrium thickens during each menstrual cycle in preparation for pregnancy. If pregnancy doesn’t occur, the tissue sheds and is expelled as menstrual blood.
However, in endometriosis, the tissue growing outside the uterus behaves in a similar way. It thickens, breaks down, and bleeds with each menstrual cycle—but because it has no way to exit the body, it becomes trapped. This trapped tissue can lead to inflammation, scar tissue (also known as adhesions), and pain.
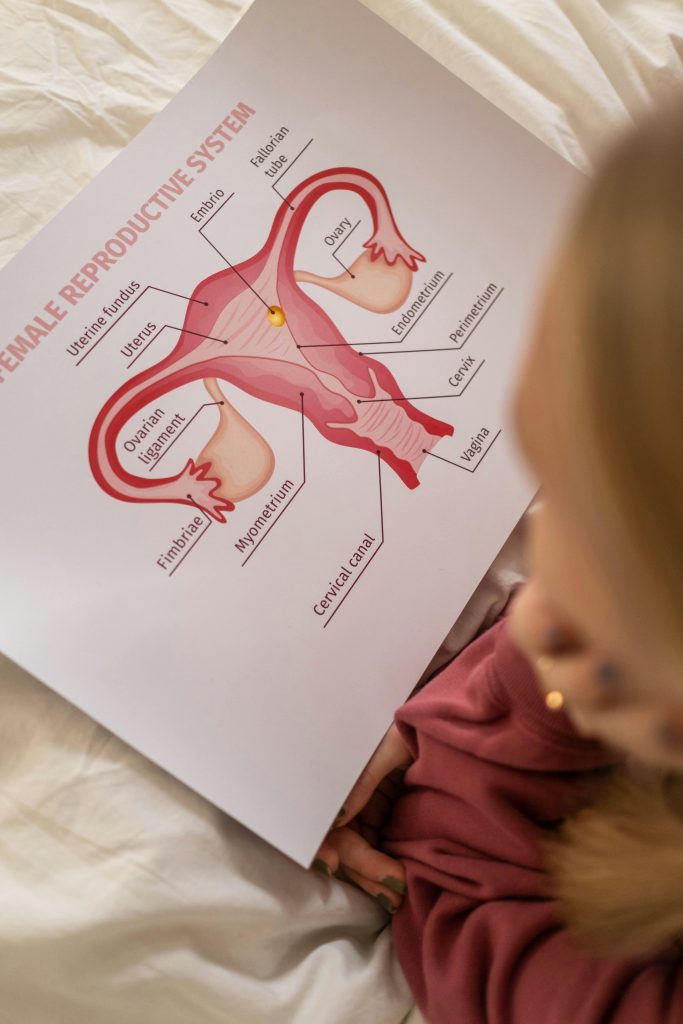
Endometriosis can affect the ovaries, fallopian tubes, and the tissue lining the pelvis. In some cases, it can spread beyond the pelvic region.
Symptoms of Endometriosis
The most common symptoms of endometriosis include:
Pelvic Pain: This is the hallmark symptom and often the most intense. It can range from dull and chronic pain to sharp and debilitating pain, especially during menstruation.
Painful Periods (Dysmenorrhea): Women with endometriosis often experience very painful periods that can get worse over time.
Heavy Menstrual Bleeding (Menorrhagia): This can include bleeding between periods or especially heavy periods that require changing sanitary products frequently.
Pain During Sex (Dyspareunia): Pain during or after intercourse is common in women with endometriosis, especially if the tissue is located near the pelvic organs.
Infertility: Around 30-40% of women with endometriosis struggle with infertility (Hickey et al., 2014). The condition can impact the fallopian tubes, ovaries, and the implantation of a fertilized egg.
Digestive Issues: Symptoms like bloating, diarrhoea, constipation, and nausea, especially around menstruation, can occur because the endometrial-like tissue can affect the intestines.
While pelvic pain is common, some women with endometriosis may have no symptoms at all, which is why it can be difficult to diagnose.
What Causes Endometriosis?
The exact cause of endometriosis is not fully understood, but there are several theories:
Retrograde Menstruation: One of the most widely accepted theories is that retrograde menstruation occurs. This is when menstrual blood flows backward through the fallopian tubes into the pelvic cavity instead of leaving the body. This can allow endometrial cells to attach and grow outside the uterus (Giudice, 2010).
Genetics: Endometriosis tends to run in families, which suggests that there may be a genetic component to the condition. If your mother or sister has endometriosis, you may be more likely to develop it yourself (Nnoaham et al., 2011).
Immune System Dysfunction: Another theory is that women with endometriosis may have a malfunctioning immune system that is unable to recognise and destroy the extra endometrial tissue growing outside the uterus (Giudice, 2010).
Embryonic Cell Transformation: Some researchers believe that during puberty, certain cells in the pelvic cavity might transform into endometrial-like tissue, a theory known as embryonic cell transformation.
How is Endometriosis Diagnosed?
Diagnosing endometriosis can be challenging because the symptoms are similar to other conditions, such as irritable bowel syndrome (IBS) or pelvic inflammatory disease (PID). However, there are several methods doctors use to diagnose the condition:
Pelvic Exam: During a pelvic exam, the doctor may feel for cysts or scars that may indicate endometriosis, but this exam is not always able to detect it.
Ultrasound: An ultrasound can help doctors identify endometriosis-related cysts, called endometriomas, on the ovaries.
Laparoscopy: This is the most definitive way to diagnose endometriosis. It is a minimally invasive surgery in which a small camera is inserted into the abdomen to directly view the endometrial tissue outside the uterus. If endometriosis is found, the surgeon may also remove or biopsy the tissue at the same time (Donnez & Donnez, 2014).
Treatment Options for Endometriosis
While there is no cure for endometriosis, several treatment options can help manage symptoms and improve quality of life. Treatment depends on the severity of the condition, symptoms, and whether the woman wants to have children in the future.
Pain Medications: Over-the-counter pain relievers like ibuprofen or naproxen can help manage mild pain. For more severe pain, doctors may prescribe stronger medications (Hickey et al., 2014).

Hormonal Therapy: Since endometriosis is oestrogen-dependent, hormonal treatments can help reduce or eliminate menstruation and slow the growth of endometrial-like tissue.
Surgery: For women with severe endometriosis or those who want to preserve fertility, surgery may be recommended. Laparoscopic surgery can remove endometriosis implants, cysts, and adhesions (Donnez & Donnez, 2014). In more severe cases, a hysterectomy (removal of the uterus) may be recommended, but this is typically a last resort.
Lifestyle and Diet Changes: Some women find relief by making lifestyle changes, such as following an anti-inflammatory diet, exercising regularly, and managing stress. While there is no one-size-fits-all approach, dietary modifications, including increased intake of omega-3 fatty acids, may reduce inflammation and improve symptoms (Zhang et al., 2018).
Living with Endometriosis
Endometriosis can be a challenging condition to live with, especially since it often goes undiagnosed for years. However, with the right treatment, many women are able to manage their symptoms and maintain a good quality of life.
It’s important for women to communicate openly with their healthcare providers about their symptoms and seek a diagnosis if they suspect they have endometriosis. Early intervention can help manage symptoms and prevent long term complications.
Endometriosis is a common, yet often misunderstood condition that affects millions of women worldwide. If you are experiencing pelvic pain, heavy periods, or difficulty with fertility, it’s important to talk to your healthcare provider about the possibility of endometriosis.
References
Donnez, J., & Donnez, O. (2014). Laparoscopic management of endometriosis. The Lancet, 383(9911), 94-97. https://doi.org/10.1016/S0140-6736(13)61871-9
Giudice, L. C. (2010). Endometriosis. New England Journal of Medicine, 362(25), 2389-2398. https://doi.org/10.1056/NEJMra0901554
Hickey, M., Ballard, K., & Micali, N. (2014). Endometriosis. BMJ, 348, g1357. https://doi.org/10.1136/bmj.g1357
Nnoaham, K. E., Hummelshoj, L., & Webster, P. (2011). Impact of endometriosis on quality of life and work productivity: A multicenter study across 10 countries. Fertility and Sterility, 96(2), 294-300. https://doi.org/10.1016/j.fertnstert.2011.05.090
Zhang, Y., Huang, L., & Cheng, M. (2018). Omega-3 fatty acids and endometriosis: A systematic review of the evidence. Reproductive Biology and Endocrinology, 16(1), 105. https://doi.org/10.1186/s12958-018-0410-3
